Immediate wound care
- Do not suck the puncture wound. Do not squeeze.
- Wash thoroughly (soap and running water) then disinfect with alcohol +/- betadine
- Document neurovascular status
- Check tetanus status
- If significant exposure take 10ml clotted blood for antigen testing and storage.
Significant Exposure
- Percutaneous injuries
- Exposure of broken skin to blood or bodily fluids
- Exposure of mucous membranes (including eye) to blood or bodily fluids
- Sexual exposure
- Human bites which breach the epidermis
Risk assessment of material
- High risk
- Blood, bodily fluids containing visible blood, semen or vaginal secretion
- Unknown risk
- CSF, synovial fluid, pleural fluid, peritoneal fluid, pericardial fluid, amniotic fluid
- Low risk
- Faeces, urine, vomitus, nasal secretions, saliva*, sputum, sweat, tears
Post Exposure Prophylaxis
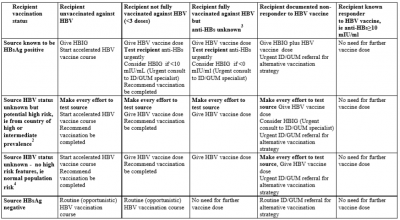
Hepatitis B Hep B prophylaxis should be offered to all patients with a significant exposure as per table opposite.
Hepatitis B vaccine is highly effective in preventing acute infection after exposure if given within 7 days and preferably within 48 hours.
Hepatitis B immunoglobulin (HBIG) is only indicated where the source is known HBsAg positive, or where the recipient is a known non-responder to HBV vaccine and the source is known to be high risk. HBIG should ideally be given within 48 hours but not later than 7 days after exposure.
Follow-up
Hospital staff should be referred to Occupational Health for follow-up. Members of the public should be referred to their GP or their own occupational Health service.
_______________________________________________________
http://www.hpsc.ie/A-Z/EMIToolkit/
Hepatitis B post-exposure prophylaxis:
1 For bite with no visible blood, risk assess or seek urgent ID specialist advice.2 Africa, Asia, South America, Central & Eastern Europe.
3 If the recipient was fully vaccinated as an infant no further no further testing or booster dose is needed. Universal infant HBV vaccination started in 2008.
4 Injecting drug users in Ireland have only a 2% risk of being HBsAg positive and are thus not considered high risk.
Post Exposure Prophylaxis HIV
HIV PEP is recommended if the source is known HIV+ with a detectable viral load and the injury is within the past 72 hrs.
HIV PEP may also be considered where the following criteria are met:
- Source is unknown but from a high prevalence group or area (e.g. needle and syringe discarded in a location where IVDUs are known to inject)
- Injury within the past 72 hrs
- There is a high likelihood that the needle has been left there in the past couple of days. In such rare circumstances, and only if all the above criteria are met, should PEP be considered. In this situation, a two-drug PEP is more appropriate, i.e. Truvada alone.
- If these criteria are not met, HIV PEP is NOT indicated.
If there is no information available about the likely source of the needle or how long it was there, PEP would not be routinely recommended, but could be discussed with the recipient & consider Truvada alone.
In cases of potential HIV exposure following sexual contact see national guidelines: http://www.hpsc.ie/A-Z/EMIToolkit/ All patients should be discussed with and followed up by Infectious Disease.
In order to streamline these referrals there are a few mandatory requirements of the ED doctor.
1. Call the ID clinic (Ext 2210) to give the patients name and state that you are referring this patient as a PEP patient. If the phone is not answered (i.e. out of hours) leave a message stating the above. The messages on this phone are checked by the ID service every morning.
2. Fill in the proforma and Fax to 091-893749 (Patient notes suffice as a referral to Fax in the interim – Obviously DOCUMENT the referral in the notes)
3. Give the patient a copy of the proforma to bring with them to the clinic.
4. Finally inform the patient that they are to attend the next ID clinic available.
ID PEP clinics are as follows:
Monday - Afternoon
Wednesday - All Day
Friday - Morning